Hysteroscopy and diagnostic endoscopy at Femcare Fertility, Kalyani Nagar, Pune allow Dr. Sayali Chavan Shitole to directly visualise and treat uterine conditions - polyps, fibroids, adhesions and septa - that cause infertility, implantation failure, or recurrent miscarriage. Consultation: ₹500.
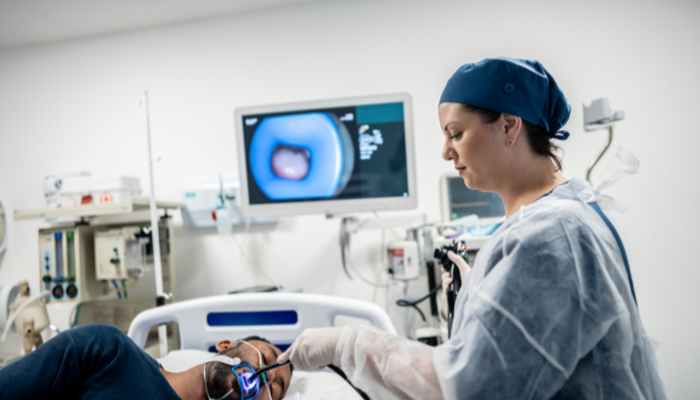
Fertility investigations can include numerous blood tests and ultrasound scans, but sometimes the most important information is only visible when a doctor looks directly inside the uterus. A 1 cm polyp that causes repeated IVF failure may not show clearly on a standard ultrasound. An intrauterine adhesion from a previous D&C might be invisible until a hysteroscope confirms it.
A fibrous septum dividing the uterine cavity - the most correctable cause of recurrent miscarriage - can be mistaken for a normally shaped uterus on 2D imaging.
At Femcare Fertility in Kalyani Nagar, Pune, Dr. Sayali Chavan Shitole uses diagnostic and operative hysteroscopy as a core diagnostic and treatment tool, not a last resort.
A hysteroscope is a thin, lighted optical instrument passed through the cervix into the uterus. No incision is required. The procedure allows the surgeon to see the uterine cavity on a screen in real time - its shape, the appearance of the lining and any abnormalities present. When treatment is needed, fine instruments are passed alongside the hysteroscope to remove polyps, cut adhesions, or resect a septum without opening the abdomen.
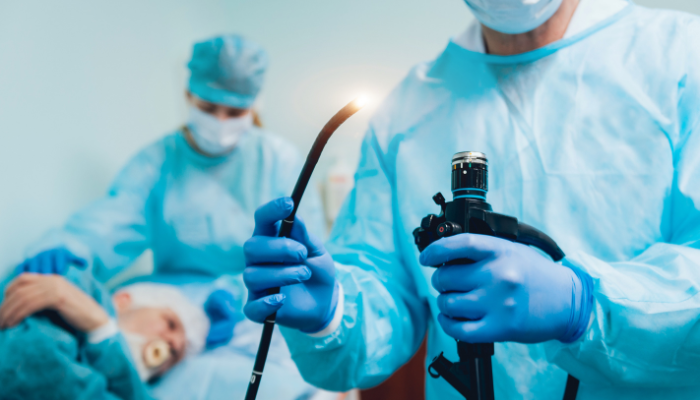
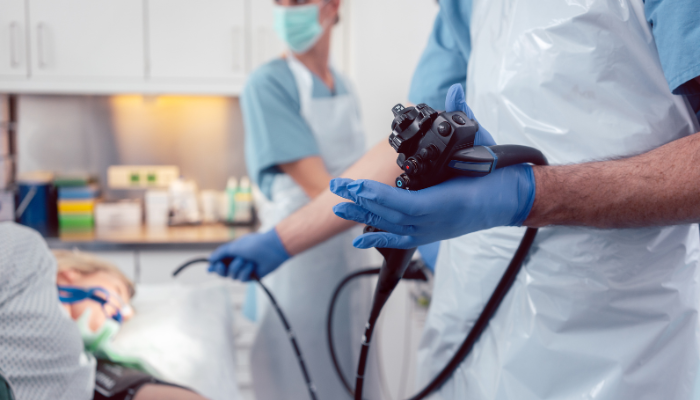
Endometrial polyps are localised overgrowths of the uterine lining. Even small polyps have been shown to reduce implantation rates in natural cycles and IVF. Their removal - a simple operative hysteroscopy - significantly improves pregnancy rates in subsequent cycles.
Submucosal FibroidsFibroids that press into the uterine cavity directly impair embryo implantation. Hysteroscopic myomectomy removes these fibroids without affecting the outer surface of the uterus, preserving fertility.
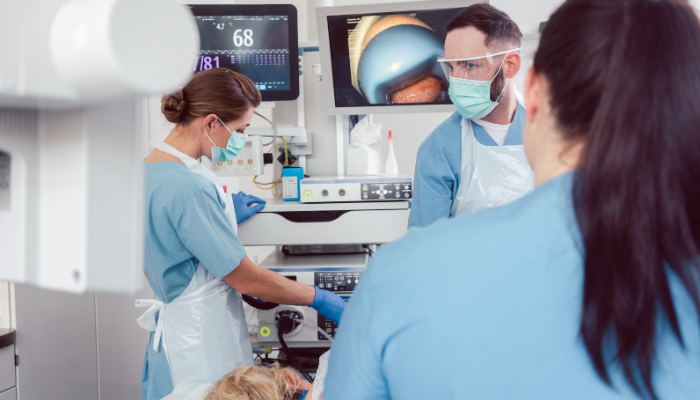
Adhesions inside the uterus - bands of scar tissue - reduce the functional area available for implantation and can cause scanty periods or amenorrhoea. Hysteroscopic adhesiolysis (cutting of adhesions) restores the cavity architecture. Post-operative oestrogen therapy encourages healthy regrowth of the endometrium.
Uterine SeptumA uterine septum is a fibrous partition dividing the cavity. It is associated with recurrent miscarriage and preterm labour . Hysteroscopic metroplasty (septum resection) is a straightforward operative hysteroscopy that corrects the shape of the cavity and reduces subsequent miscarriage rates.
When diagnostic work-up suggests both uterine and pelvic pathology - for example, a possible septum AND possible endometriosis - Dr. Sayali may perform combined laparoscopy and hysteroscopy under the same general anaesthetic. This approach addresses both the inside and outside of the uterus in one admission and reduces the total number of procedures a patient needs.
Dr. Sayali performs hysteroscopy before IVF in women who have had a previous uterine procedure, women with unexplained previous implantation failure and where an ultrasound finding requires clarification. This increases the confidence that the uterine cavity is ready for embryo transfer.